Call Us Today!
(631) 821-2244

Dry Eye is a common disease affecting vision quality and eye comfort. Symptoms of Dry Eye can vary widely from patient to patient. People with Dry Eye may experience one or more of the following symptoms:
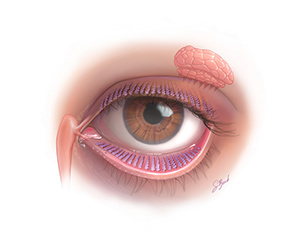
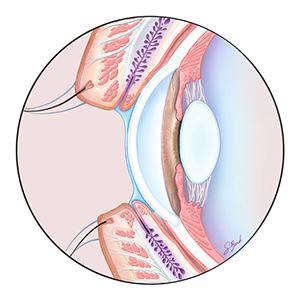
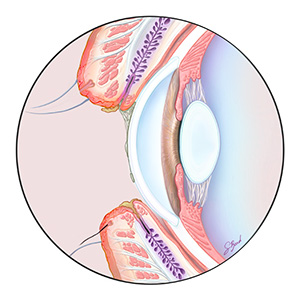
At our clinic, we use a number of different technologies to determine whether you may be experiencing Dry Eye and to better understand your symptoms. Dry Eye is a serious condition that can dramatically affect your vision and your eye health.
Dry eye can be influenced by a number of factors related to environment and health that determine tear quality.
Tears have 3 layers:
If there’s an imbalance in these layers, your vision and comfort of your eyes may be affected. For example, if not enough lipid layer is being produced, tears may evaporate too quickly and cause symptoms ranging from discomfort to extra tear production and poor quality of vision.
Poor tear quality is often caused by Meibomian Gland Dysfunction (MGD), a condition that impacts the production of oils in your tears. The most common form of MGD is obstruction of the oil producing glands in the eyelids. At Soundview Eye Center, we will test your tear quality to determine whether MGD is contributing to or causing your dry eye symptoms and create a customized treatment plan to address it.
Each case of Dry Eye is unique. We consider the factors causing your dry eye as well as your tear quality to develop a custom dry eye treatment plan.
Management considerations for Dry Eye include artificial tears/lubricant drops which provide short-term relief of symptoms. Other options include prescription anti-inflammatory drops and in-office obstruction removal with medical devices like The TearCare® System.

TearCare® is an innovative Dry Eye procedure that targets the blocked meibomian glands in your eyelids that produce oils to keep your tears healthy. When these glands become blocked or have reduced function, your tears may evaporate more quickly. Unblocking these glands with The TearCare® System can help restore their function and stabilize the tear film. This may improve the quality of tears and reduce symptoms like dryness, gritty or scratchy sensations, blurry vision, and watery eyes.
At your appointment, we will determine whether your dry eye symptoms are caused by Meibomian Gland Dysfunction (MGD) and would benefit from the use of The TearCare® System.
TearCare® is an in-office treatment designed to address dry eye caused by meibomian gland dysfunction (MGD). The system uses small, wearable thermal devices applied to the outer eyelids to deliver controlled heat that softens hardened oils in the glands. After heating, the clinician expresses the glands to remove blockages and help restore natural oil flow.
Improving oil secretion helps stabilize the tear film by reducing tear evaporation and improving lipid layer quality. The procedure is performed with topical anesthetic and is intended to work with the eye’s natural anatomy rather than replace normal gland function. A full dry eye evaluation is used to determine whether TearCare® is an appropriate option for each patient.
Good candidates are patients who show signs of meibomian gland dysfunction and symptoms such as dryness, burning, grittiness, fluctuating vision or excessive tearing. Diagnostic testing that evaluates tear quality and gland structure helps identify whether blocked or poorly functioning glands are contributing to symptoms. Candidates should have realistic expectations and be willing to follow recommended follow-up care and home routines.
TearCare® is typically considered when conservative measures like lid hygiene and artificial tears provide incomplete relief. It may be recommended for patients with chronic or recurrent MGD who need targeted gland clearance. Your clinician will review medical history and exam findings to confirm that TearCare® is suitable for your specific condition.
During a TearCare® visit you will be seated while the clinician places the soft devices across the outer eyelids and secures them with an adhesive mechanism. The devices deliver precise thermal energy for a predetermined time while you remain comfortable and awake. After the warming phase, the clinician performs manual gland expression to evacuate liquefied oils and clear obstructions.
The full appointment includes diagnostic testing, the procedure itself and a brief post-procedure assessment to ensure comfort. Topical anesthetic is commonly used to minimize any sensation during expression. Most patients report only mild transient discomfort and can resume normal activities immediately after the visit.
A typical TearCare® appointment usually takes between 20 and 40 minutes, depending on the extent of testing and the number of lids treated. The heating phase lasts a set interval and is followed by gland expression and a short clinical assessment. Most of the time is spent on evaluation and ensuring proper gland clearance rather than lengthy procedural steps.
There is minimal recovery time associated with TearCare®, and patients commonly return to regular activities right away. Some people may experience mild, short-lived irritation, tearing or itchiness that resolves within hours to a day. Your clinician will provide post-procedure guidance on eye care and any temporary activity modifications.
Many patients notice symptomatic improvement within days to weeks as gland secretions normalize and the tear film stabilizes. Early changes may include reduced grittiness, less burning and more consistent vision between blinks. The timeline varies by individual and by how long glands have been obstructed prior to treatment.
Objective improvements in tear quality and gland function may be tracked over several follow-up visits to document progress. Some patients require adjunctive therapies or repeat treatments to achieve and maintain optimal results. Your clinician will discuss expected timelines based on your exam findings and treatment response.
Duration of benefit varies; many patients experience meaningful relief for several months to a year following a single treatment, while others may need maintenance at intervals determined by symptom recurrence and gland health. Meibomian glands can re-occlude over time, especially if underlying contributing factors remain unaddressed. Maintenance plans are individualized and based on clinical response and patient needs.
Periodic follow-up exams help the clinician determine the timing of potential repeat treatments and any adjunctive therapy. Combining in-office care with consistent lid hygiene and recommended at-home measures can extend the interval between procedures. Your provider will explain a tailored plan to help preserve gland function and tear quality.
TearCare® is generally well tolerated, but like any medical procedure it carries potential risks that are typically mild and transient. Possible short-term effects include increased tearing, slight eyelid irritation, redness or temporary visual fluctuation that resolve within hours to a few days. Serious complications are uncommon when the procedure is performed by trained clinicians following established protocols.
Before treatment your clinician will review your medical history and discuss expected benefits and risks so you can make an informed decision. If you have eyelid skin conditions, active infection or other ocular issues those factors will be considered and managed appropriately. Prompt follow-up is recommended for any unexpected or persistent symptoms after the procedure.
TearCare® specifically targets meibomian gland obstruction with controlled eyelid warming and manual expression, which differs from treatments that focus primarily on surface lubrication or inflammation control. Artificial tears and ointments provide symptomatic relief but do not address clogged glands; prescription anti-inflammatory drops may reduce surface inflammation but may not clear gland obstructions. TearCare® is part of a spectrum of therapies and is chosen when gland dysfunction is a key driver of dry eye symptoms.
Other in-office options, such as intense pulsed light or manual gland expression alone, have different mechanisms and evidence profiles, and the ideal approach depends on the individual patient’s exam findings. Your clinician will review the advantages and limitations of each modality and recommend a plan that best targets the causes identified during your evaluation. Combining complementary therapies is often the most effective strategy for long-term management.
Preparation is minimal but important for an efficient visit: bring a list of current eye medications, wear no eye makeup, and avoid eyelid creams or oils on the day of the procedure. If you wear contact lenses, you may be asked to remove them before testing and the treatment itself. Plan for a short appointment window and consider arranging transportation if you prefer not to drive immediately after a procedure, although most patients can drive home.
At Soundview Eye Center your provider will perform a dry eye evaluation to confirm candidacy and explain the steps of the procedure, expected sensations and aftercare instructions. Communicate any history of eyelid or skin conditions, recent ocular infections, or systemic health issues during your intake. Clear communication helps ensure a safe, personalized treatment experience.
Yes, TearCare® is often integrated into a comprehensive dry eye management plan that may include lid hygiene, warm compresses, artificial tears, dietary modifications and prescription medications when indicated. Treating MGD directly with TearCare® can improve the effectiveness of other measures by restoring healthier gland secretions. A multimodal approach addresses both gland dysfunction and surface inflammation for more durable symptom control.
Your clinician will tailor a combination of in-office and at-home therapies based on diagnostic findings and treatment response. Follow-up visits are used to monitor progress, adjust therapies and determine whether additional in-office care is needed. Consistent adherence to the recommended plan supports better long-term outcomes.
