Call Us Today!
(631) 821-2244
Glaucoma is a group of eye conditions that damage the optic nerve, the critical pathway that carries visual information from the eye to the brain. Damage usually occurs gradually and can begin long before symptoms are noticeable. In many cases, peripheral (side) vision is affected first, and by the time central vision is impaired a person may have already experienced significant, irreversible loss. Because of this stealthy nature, glaucoma is often called a "silent" disease.
There are several forms of glaucoma, including primary open-angle glaucoma, angle-closure glaucoma, and secondary glaucomas related to other eye conditions or medications. Each type has distinct features, but they share the common mechanism of optic nerve injury. Elevated intraocular pressure (IOP) is a major risk factor and a primary target for treatment, but people can also develop glaucoma with normal IOP levels; the overall health of the optic nerve and its blood supply matters greatly.
Understanding the disease is the first step toward protecting sight. Awareness that glaucoma often progresses without pain or early symptoms underscores the importance of routine eye examinations. Early detection allows for interventions that slow—or in many cases, halt—further damage, preserving vision and maintaining quality of life.
Glaucoma risk increases with age, family history, and certain medical conditions such as diabetes and hypertension. People of African, Hispanic, and Asian descent may face higher risks for particular forms of the disease, and previous eye injuries, long-term steroid use, and certain anatomical features of the eye can also contribute. Because risk varies between individuals, a personalized approach to screening is essential.
Routine eye care includes specific tests designed to identify early signs of glaucoma before noticeable vision loss occurs. For many patients, regular monitoring of intraocular pressure and inspection of the optic nerve during comprehensive eye exams will be sufficient. Those with higher risk profiles may need more frequent evaluations and specialized diagnostic testing to catch subtle changes as early as possible.
Early detection not only preserves vision but also provides more flexible treatment options. When glaucoma is found at an early stage, less invasive therapies are often effective at maintaining eye health. Encouraging patients to maintain scheduled exams—particularly if they fall into a higher-risk group—is one of the most effective strategies for preventing serious vision loss.
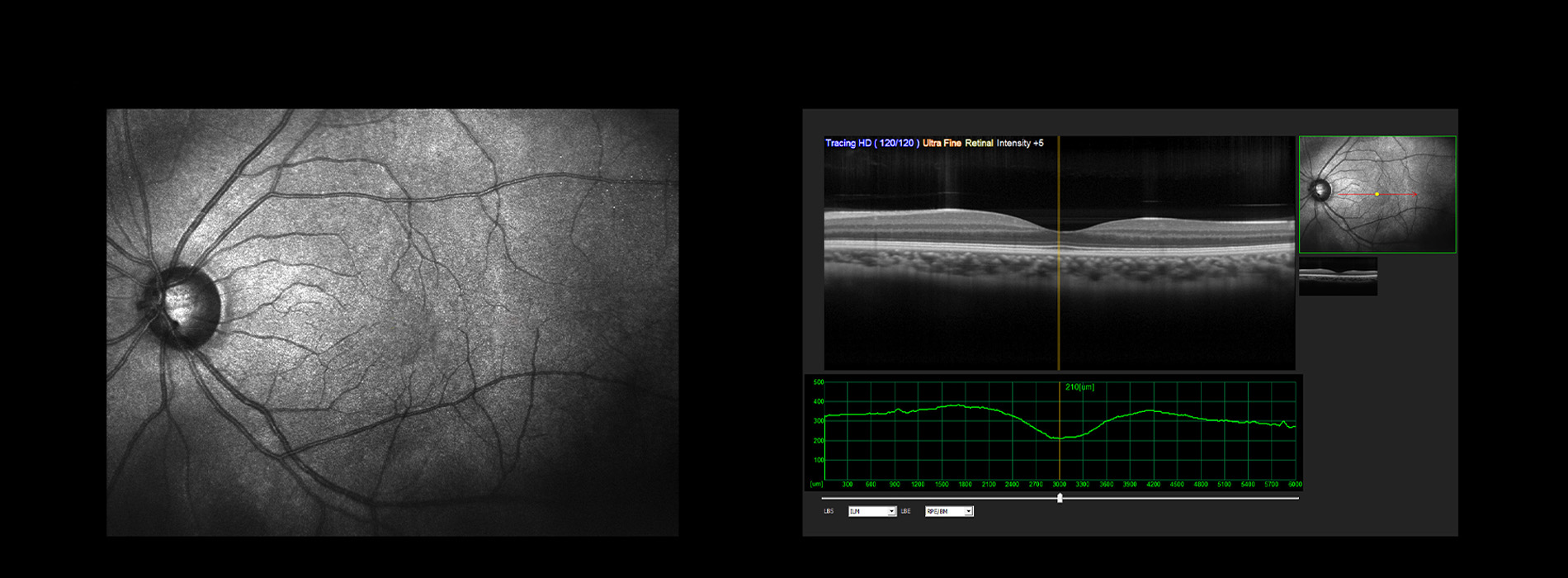
Today's ophthalmic testing goes well beyond a basic vision check. Tonometry measures intraocular pressure, but that measurement is only one piece of the puzzle. A thorough evaluation also includes detailed inspection of the optic nerve head using slit-lamp biomicroscopy and imaging technologies that capture cross-sectional and surface views of the nerve and retinal layers. These objective images allow clinicians to document subtle structural changes over time.
Visual field testing is another cornerstone of glaucoma assessment. It maps peripheral vision and identifies functional deficits that may not be noticeable to the patient. Automated perimetry provides repeatable, quantifiable results that help track progression and guide treatment decisions. In many practices, optical coherence tomography (OCT) is used to measure the thickness of retinal nerve fiber layers and the optic nerve, often revealing damage before visual field loss becomes apparent.
Collectively, these diagnostic tools give eye care professionals a detailed picture of both structure and function, improving the accuracy of diagnosis and allowing earlier, more tailored interventions. When combined with a patient’s medical history and risk profile, testing results form the basis for a sensible, evidence-based management plan.
Treatment for glaucoma aims to slow or stop optic nerve damage and protect remaining vision. The mainstay of initial therapy is typically topical medications that lower intraocular pressure; these are carefully selected based on the patient’s overall health, lifestyle, and ocular characteristics. For patients who cannot tolerate or adequately respond to medications, laser procedures offer a minimally invasive alternative that can reduce pressure and, in some cases, decrease dependence on eye drops.
When disease progresses despite less invasive measures, surgical options are available that create new pathways for fluid drainage or otherwise reduce pressure inside the eye. Advances in microinvasive glaucoma surgery (MIGS) have expanded choices for earlier surgical intervention with a favorable safety profile for appropriate candidates. The choice among drops, lasers, and surgery is individualized: the goal is to balance effectiveness, safety, and the patient's preferences.
Effective glaucoma care is a partnership. Treatment plans are regularly reviewed and adjusted in response to test results and the patient’s day-to-day experiences. Medication adherence, awareness of side effects, and open communication with the care team are essential components of successful long-term management.
Because glaucoma is typically chronic, ongoing monitoring is essential. Patients diagnosed with glaucoma or identified as glaucoma suspects require a schedule of follow-up exams that may include pressure checks, optic nerve imaging, and visual field testing. These visits are not merely administrative—they’re opportunities to detect progression early and to alter therapy in a timely manner to protect vision.
Lifestyle factors can influence eye health and support clinical treatment. Maintaining a healthy overall medical profile, managing chronic conditions such as diabetes and high blood pressure, avoiding smoking, and following prescribed medication regimens all contribute to better outcomes. In addition, patients should report any sudden symptoms—such as eye pain, rapid vision changes, or severe redness—to their eye care provider promptly.
At Soundview Eye Center, our approach to glaucoma management combines the latest diagnostic technology with personalized care plans designed to preserve vision and maintain quality of life. We work closely with each patient to explain findings, set treatment goals, and schedule the necessary follow-up to keep disease progression under control. Our objective is to empower patients with information and care that reduce the risk of future vision loss.
If you're concerned about glaucoma because of symptoms, family history, or risk factors, early evaluation can make a meaningful difference. Regular exams and consistent follow-up are the best defenses against the long-term consequences of the disease. Contact us to learn more about glaucoma screening, testing options, and how we can help you manage your ocular health.
Glaucoma is a group of eye conditions that damage the optic nerve, which transmits visual information from the eye to the brain. Damage most often progresses slowly and begins with peripheral vision loss, so many patients do not notice changes until the disease is advanced. Because early stages are frequently symptomless, regular eye exams are essential for timely detection.
Not all glaucoma is associated with high pressure, but lowering intraocular pressure is the primary focus of most treatments because it reduces stress on the optic nerve. Over time, untreated glaucoma can cause irreversible vision loss and interfere with daily activities. Early diagnosis and ongoing monitoring give clinicians the best chance to preserve sight.
Risk increases with age, a family history of glaucoma, certain medical conditions such as diabetes and hypertension, a history of eye injury, long-term steroid use, and specific anatomic features of the eye. People of African, Hispanic and Asian descent are more likely to develop particular types of glaucoma and should be especially vigilant about screening. Your personal risk profile determines how aggressively the eye care team will monitor you.
Screening frequency is individualized based on risk factors and prior test results; some patients benefit from annual exams while others need testing every few years. Patients with suspicious findings or a confirmed diagnosis usually require more frequent follow-up to detect changes early. Your clinician will recommend a schedule that balances thorough monitoring with your lifestyle and medical needs.
A comprehensive glaucoma evaluation combines measurements of intraocular pressure with inspection of the optic nerve, optical imaging and visual field testing. Tonometry assesses eye pressure, slit-lamp and dilated optic nerve exams reveal structural changes, optical coherence tomography (OCT) measures nerve fiber and retinal layer thickness, and automated perimetry maps peripheral vision. Pachymetry, gonioscopy and photographic documentation may also be used to build a reliable baseline for comparison over time.
These tests work together to capture both structural and functional information so clinicians can identify subtle progression before significant vision loss occurs. Repeating the same tests over time allows practitioners to distinguish true change from normal variability. High-quality baseline data are essential for making confident treatment decisions and tracking long-term outcomes.
Treatment decisions are individualized and based on a combination of test results, the rate of progression, the patient’s overall health and personal preferences. Clinicians establish a target intraocular pressure tailored to the degree of optic nerve damage and adjust therapy to reach and maintain that goal. The decision-making process balances expected benefits, potential side effects and the patient’s ability to follow the regimen.
Good glaucoma care is a partnership that relies on clear communication about risks, possible side effects and practical issues such as adherence. If a therapy is ineffective or poorly tolerated, clinicians reevaluate and consider alternatives such as laser procedures or surgery. Regular reassessment ensures the plan remains aligned with clinical findings and patient needs.
The primary goal of glaucoma treatment is to lower intraocular pressure to a level that slows or stops optic nerve damage. First-line therapy often includes topical medications that either decrease fluid production in the eye or improve drainage, and these drops are selected based on efficacy, side effect profile and patient lifestyle. Laser procedures such as selective laser trabeculoplasty can reduce pressure by improving outflow and are commonly used when drops are insufficient or adherence is an issue.
When drops and lasers do not adequately control the disease, surgical options create new drainage pathways or enhance existing ones to reduce pressure long-term. Advances in microinvasive glaucoma surgery (MIGS) have increased the options for many patients by offering less invasive alternatives with a favorable safety profile in appropriate cases. The choice of therapy depends on disease severity, anatomical considerations and the patient’s treatment goals.
Surgery is considered when glaucoma progresses despite medical and laser treatments, when patients cannot tolerate medications, or when long-term medication use is impractical. The specific procedure recommended depends on disease severity, eye anatomy and prior surgeries, and the goal is to achieve a stable, lower intraocular pressure while minimizing complications. Your eye care team will explain risks, benefits and expected recovery so you can make an informed decision.
Options range from microinvasive glaucoma surgery (MIGS), which can be appropriate for earlier stages and is often combined with cataract surgery, to more traditional procedures such as trabeculectomy or tube shunt implantation for advanced or refractory disease. Each approach has different efficacy and safety profiles, and selection is personalized to the patient’s clinical situation. Close postoperative follow-up is important to monitor healing and long-term pressure control.
Follow-up frequency is individualized and depends on the severity of disease, rate of progression and the stability of test results. Patients with early, well-controlled glaucoma may be seen every three to six months, while those with rapid progression or unstable findings often require more frequent visits and testing. Newly diagnosed patients or those undergoing treatment changes typically have closer monitoring until the response is clear.
Consistent follow-up permits timely adjustments to therapy and helps detect subtle changes that could threaten vision. Your clinician will set a schedule for intraocular pressure checks, imaging and visual field testing based on current findings and risk factors. Adhering to that plan gives the best chance of preserving long-term vision.
While medical and surgical treatments are central to glaucoma care, certain lifestyle measures support overall eye health and may help complement clinical therapy. Maintaining good control of systemic conditions such as diabetes and hypertension, avoiding smoking, getting regular moderate exercise and following a balanced diet all contribute to vascular and optic nerve health. Adequate sleep and stress management may also play a supportive role in general well-being.
Patients should take prescribed eye medications consistently and learn correct drop administration to maximize benefit. Protective eyewear during activities that risk eye injury and prompt reporting of symptoms such as sudden vision changes, severe eye pain or marked redness are also important. These practical habits, combined with regular clinical follow-up, enhance the effectiveness of professional care.
Many patients do not notice early progression because peripheral vision loss can be subtle, which is why objective testing is the primary method of detecting deterioration. Changes on OCT imaging, worsening visual field test results, or documented structural decline of the optic nerve are signs that therapy may need to be intensified. Your clinician will compare current exams with prior baselines to determine whether true progression has occurred.
If progression is identified, the care team will consider stepping up treatment by adjusting medications, recommending laser therapy, or discussing surgical options depending on the pace and extent of change. The goal is to slow or halt further damage and preserve remaining vision, and decisions are guided by the severity of progression and the patient’s overall health. Timely communication and adherence to follow-up are key to responding effectively to progression.
At Soundview Eye Center we combine comprehensive diagnostic testing with individualized treatment plans to preserve vision and maintain quality of life for each patient. Our approach emphasizes establishing a clear baseline with imaging and visual field testing, setting personalized target pressures, and communicating treatment options so patients can participate in decisions about their care. We prioritize regular monitoring and timely adjustments to therapy based on objective findings.
The practice also coordinates care with surgical colleagues when advanced interventions are appropriate and educates patients about adherence, symptom recognition and lifestyle strategies that support treatment. By integrating technology, evidence-based protocols and patient-centered communication, our team aims to deliver reliable, long-term glaucoma management. Patients are encouraged to contact the office with concerns and to maintain scheduled follow-up to protect their vision.
